Food Allergies in Babies and Toddlers: Symptoms, Diagnosis, and Treatment Guide
With good care, children with food allergies can grow, thrive, and live healthy, active lives. Some babies may even outgrow their allergies as they get older, which gives families hope for the future. Your baby’s pediatrician or a pediatric allergist can guide and support you.
At-a-Glance: Food Allergies in Babies and Toddlers
- Food allergies occur when a baby’s immune system mistakenly treats certain foods as dangerous threats. In response, the body releases histamine. This causes symptoms ranging from mild skin hives to life-threatening anaphylaxis. Infant allergies, including food allergies, can arise at any age, even in the youngest children.
- Nine foods cause 90% of reactions. These are: milk, eggs, peanuts, tree nuts, soy, wheat, fish, shellfish and sesame. Since babies can’t tell you what they’re feeling, parents must watch for subtle changes in skin, breathing, behavior and digestion. The prevalence of food allergies in U.S. children is about 8%. Nearly 3% of U.S. infants develop a food allergy in the first year of life.
- Diagnosis requires more than just testing. Pediatric allergists combine skin prick tests or blood tests with your baby’s symptom history. They may also conduct an oral food challenge.
- Strict allergen avoidance. It’s important to read food product labels every time. (Ingredients can change without warning.) Prevent cross-contact through careful cleaning and teach all caregivers to recognize reactions.
- Epinephrine is the only medication that stops anaphylaxis. Always carry two doses. Be sure you know how to use the product and when to administer it. (Epinephrine auto-injectors are approved for infants if the child weighs 16.5 pounds or more.) You should give it immediately when symptoms appear to affect multiple body systems or are severe in any single system.
- Some babies outgrow certain allergies by age 3-5. Regular follow-ups with your pediatric allergist help you to track progress through repeat testing. The process may reveal when it’s safe to reintroduce foods through supervised oral challenges.

What is a Food Allergy in Babies?
A food allergy can happen when a baby’s immune system reacts to a food as if it is harmful, even though the food is normally safe. The immune system is supposed to protect the body from germs and illness. With a food allergy, it makes a mistake and treats certain food proteins like a threat.
Most food allergies in babies are caused by an immunoglobulin E (IgE)-mediated immune reaction. This means the body develops a special allergy antibody called IgE to that food. When the baby eats that food, the immune system releases chemicals such as histamine. These chemicals cause allergy symptoms, which may range from mild to very serious.
In babies, symptoms may include hives, swelling, vomiting, diarrhea, coughing, wheezing, or trouble breathing. Most allergic reactions happen within minutes to two hours after eating the food. (Some delayed reactions can happen later, especially digestive symptoms. But these may involve different immune pathways.)
Because babies can’t tell you how they feel, parents and caregivers play an important role. Watching for changes in your baby’s skin, breathing, behavior, or feeding helps you recognize symptoms early and get the care your baby needs. With the right support and medical guidance, most families learn to manage food allergies safely and confidently.
Food allergy vs. food intolerance in babies
Babies and toddlers can have a food allergy and/or a food intolerance. A food allergy involves the immune system and can be life-threatening if symptoms are severe. A food intolerance only affects digestion and is not life-threatening. Cow’s milk (lactose) is the most common food intolerance in babies. Symptoms of food intolerance may include tummy discomfort, reflux, nausea, diarrhea, cramping and gas.
Common Food Allergens in Babies and Toddlers
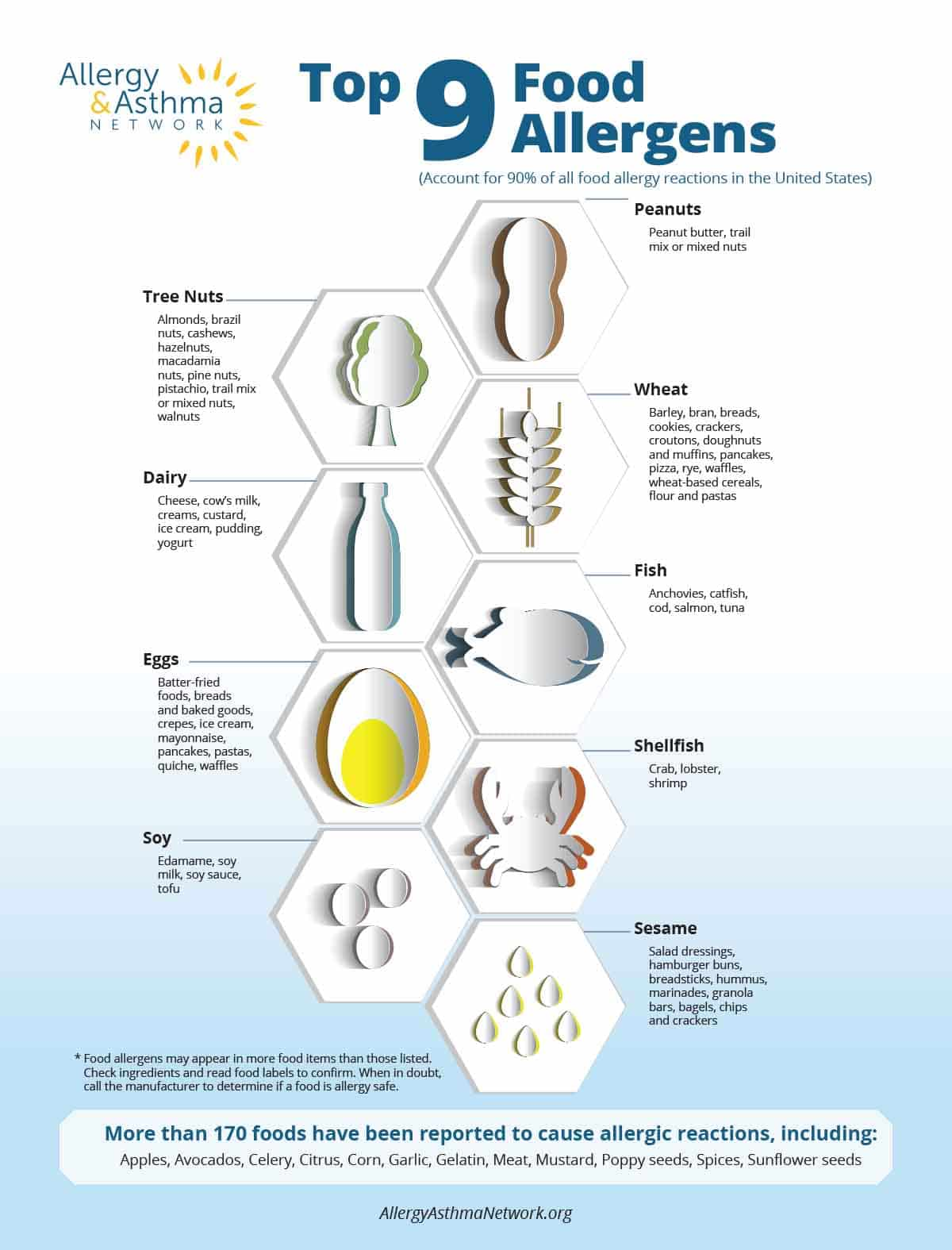
Babies can be allergic to any food. But nine allergens account for 90% of all food allergy reactions in young children.
Top 9 food allergens:
- Milk
- Eggs
- Peanuts
- Tree nuts
- Soy
- Wheat
- Fish
- Shellfish
- Sesame
Milk, eggs, peanuts, soy, wheat, tree nuts, fish and shellfish are the most common food allergens found in babies.
Allergies to milk, egg, wheat and soy often resolve in childhood. But they can persist longer or become lifelong in some people.
It’s important to monitor your baby for reactions anytime you are introducing new foods into the diet. It’s important to not avoid these foods unnecessarily, though. Research shows that early introduction of common allergens can help prevent allergies from developing in the first place. Talk with your child’s food allergy doctor about introducing new solid foods into your baby’s diet, especially if there’s a history of food allergies in family members.

Food Allergy Symptoms in Babies and Toddlers
Food allergy symptoms can look different in babies compared to older children and adults. Since babies can’t explain what they’re feeling, parents and caregivers must be alert to subtle signs of a reaction.
Reactions can be hard to spot. They may vary from child to child. Some are mild, while others can become severe quickly and lead to anaphylaxis. This makes learning the early warning signs an essential step in keeping your baby safe.
Mild symptoms (in one body system):
- A few hives on the skin
- Scratching or rubbing skin
- Itchy nose or sneezing
- Itchy mouth
- Eye rubbing or itching
- Stomach nausea or discomfort
- Tongue thrusting or pulling
- Putting fingers in the ears
- Repetitive lip licking or licking of hands or objects
- Spit-up that is more intense than normal
- Arching of the back or putting knees to the chest
Severe symptoms (affecting one or more body systems):
- Skin. Many hives over the body. Hives that appear red on light skin or look darker, purplish or blend with skin ton in babies with skin of color. Obvious swelling on the face.
- Breathing. Shortness of breath, wheezing or coughing. Tight or hoarse throat. Trouble breathing or swallowing. Swelling of lips or tongue that impacts breathing. Belly breathing (stomach moving up and down). Fast breathing. Nasal flaring. Barky or croup-like cough.
- Heart. Pale or bluish skin color. Weak pulse. Fainting or dizziness. Mottled skin (discolored patches). Pale appearance in light skin, dusky appearance in darker skin, particularly on the lips, tongue or gums.
- Stomach. Vomiting more than once. Large amounts of diarrhea.
- Neurologic (behavior). Very tired or difficult to wake up. Withdrawn. Unexpected crankiness. Inconsolable crying.

What is Anaphylaxis in Babies?
Anaphylaxis is a medical condition that occurs when symptoms of a food-allergic reaction become severe. It can be life-threatening. Anaphylaxis is rare in infants and toddlers, but it can happen – and requires immediate treatment with epinephrine. Young children usually respond very well when treated quickly.
How does anaphylaxis in infants happen? Your baby’s immune system overreacts to a food allergen that it mistakenly sees as harmful. The immune system then releases a rush of histamine and other chemicals. This can cause sudden inflammation on different parts of the body. Symptoms may involve the skin, heart, stomach, and airways.
In babies, anaphylaxis can start within minutes after eating a food allergen. Symptoms usually affect two or more body systems, or get worse very quickly in one body system. Anaphylaxis is a medical emergency and should be treated right away with epinephrine, the first-line treatment. Epinephrine is the only medication proven to stop anaphylaxis. It is approved for babies and toddlers who weigh at least 16.5 pounds. The dose is .1 mg. The auto-injector AUVI-Q® is the only epinephrine product available for young children at that weight, and learning about different routes of administration of epinephrine for anaphylaxis can help you plan for emergencies as your child grows.
With the right knowledge and awareness of infant anaphylaxis, parents and caregivers can act fast and keep children safe, and short explainer videos on recognizing and treating anaphylaxis can reinforce what to do in an emergency.
When to treat your baby with epinephrine
If a severe allergic reaction occurs and is clearly present in one or more body systems, treat with epinephrine and follow your child’s emergency care plan.
For mild allergic reactions, discuss treatment with your doctor. However, if mild symptoms are present in more than one body system, treat with epinephrine and follow your child’s emergency care plan.

How Babies Can be Exposed to Food Allergens
Your baby can come into contact with allergens in one of several ways. Understanding these exposure routes is key to recognizing early signs of serious reactions and managing infant anaphylaxis and food allergies if they occur:
- Eating the food (oral ingestion). This is the most common way allergic reactions happen. Always read food labels carefully every time you shop or check menus in restaurants.
- Touching the food (skin contact): Getting an allergen on your baby’s skin may cause a rash or hives where the allergen touched. If your baby then touches the eyes, nose or mouth, it could lead to a more serious reaction.
- Cross contact: This happens when an allergen accidentally transfers to a safe food through shared utensils, countertops or hands.
- Breathing it in (inhalation): This is very rare, but it can happen when crushed powders are in the air or cooking fumes contain airborne food particles.
Diagnosing Food Allergies in Babies and Toddlers
If you think your baby may have a food allergy, your pediatrician is usually the best place to start. The pediatrician can review symptoms and provide guidance. You may be referred to a pediatric allergist. These are food allergy specialists who can help diagnose and treat allergies in children. They understand the unique needs of infants and toddlers.
It may also be helpful to track your baby’s reactions in a food and symptom diary:
- When did the reaction occur?
- How often do the reactions occur?
- What foods triggered the reactions?
Provide this information to the pediatrician or pediatric allergist to help make the diagnosis more accurate.
The diagnosis process
Doctors diagnose food allergies using the following tools:
Oral food challenge. The doctor will give your baby a very small amount of food, then increasingly larger amounts, to see if allergy symptoms develop. This is the most accurate food allergy test. It should only be done under medical supervision in a clinic.
Medical and family history. What foods has your baby eaten? When did symptoms appear? Has your baby eaten the food before without problems? Do other family members have food allergies?
Allergy testing. Skin tests and blood tests can show if your baby’s body develops allergy antibodies to certain foods.
Test results alone do not confirm a food allergy diagnosis. Doctors will combine your baby’s test results with your baby’s history of symptoms to make a diagnosis.
Food Allergy Testing for Infants
Doctors use three types of tests to diagnose a food allergy.
Skin test in infants
During a skin test, a tiny drop of food extract is placed on the skin. Then the skin is gently pricked so that the liquid can get inside. If a bump (a wheal) appears within 15-20 minutes, the doctor will measure it. The size of the bump helps show if there is an allergy to that food.
When performed by an allergist in a medical setting, skin testing is safe and well-tolerated for infants, including those with mild eczema. Keep in mind that a positive test doesn’t always mean a true allergy. It may show sensitization instead.
Specific IgE blood tests
An IgE blood test uses a small blood sample to measure the level of food-specific IgE. If IgE numbers are high, it might mean your baby has a food allergy. The numbers on the test do not reveal how bad a reaction could be. For a more complete diagnosis, the blood test should be combined with your child’s health history and family history.
Component blood test
A component blood test takes a blood sample and checks for IgE antibodies against specific parts of a food. For example, some babies react to proteins in raw eggs but can safely eat baked eggs. A component test tells the allergist which parts of the food cause a reaction.
Oral food challenge
An oral food challenge is the most accurate test (called the “gold standard”) for diagnosing a food allergy. It can confirm a food allergy diagnosis in any age group and evaluate the potential severity of allergic reactions.
How it works: under medical supervision in a clinic, your baby eats a very small amount of a suspected food allergen. If there is no reaction, the amount of food is gradually increased over several steps. The doctor monitors your baby for signs of an allergic reaction, like skin hives, breathing problems or stomach upset.
Because an oral food challenge involves exposing a patient to a potential food allergen, there is still a risk of a serious systemic reaction. Epinephrine and other emergency treatments should be readily available at the clinic.
Important: do not attempt an oral food challenge at home. It should only be done under medical supervision in a clinic.

Conditions that Look Like Food Allergies
Certain medical conditions may have similar symptoms to food allergies. Other medical conditions may exist alongside food allergies. This can make it more challenging to determine if a child is developing food allergy or experiencing another issue.
FPIES (food protein-induced enterocolitis syndrome)
FPIES causes severe vomiting (main symptom), diarrhea, and belly pain 1-4 hours after eating. It’s a non-IgE reaction, so skin and blood tests won’t detect it. The most common triggers are milk (including infant formula), soy, rice, oats and grains. Doctors diagnose FPIES by monitoring symptoms. They may also conduct an oral food challenge.
There is no cure for FPIES. After finding out which food is the trigger, it’s very important for children with FPIES to avoid that food completely. Parents should work with a doctor and dietitian to develop a personalized diet plan that ensures proper nutrition.
Eczema (atopic dermatitis)
Food allergy symptoms and eczema can sometimes look a lot alike. This can be confusing for parents. Both conditions can cause dry, itchy skin. Your baby may rub or scratch the affected skin, or seem uncomfortable. Rashes may show up on the cheeks, arms, legs or tummy, and it can be hard to know what is causing it.
Sometimes, a food allergy can make eczema worse. After a baby eats a food they are allergic to, their body may react. This can lead to more itching, swelling or a flare-up of eczema patches. These changes may happen right away or a few hours later.
If you think food may be making your baby’s eczema worse, talk with your pediatrician or an allergist. Do not remove important foods from your baby’s diet without talking to a doctor first, because babies need good nutrition to grow and stay healthy.
When a baby’s eczema progresses to food allergies, asthma or allergic rhinitis, it’s called the allergic march. Babies with early eczema are at higher risk for the atopic march, so doctors tend to watch closely for signs of allergic conditions as the child grows.
Other conditions that can be mistaken for food allergies
- Viral infections that cause skin rash
- Eosinophilic esophagitis (EoE) – inflammation in the esophagus that causes swallowing problems
- Celiac disease – an autoimmune condition triggered by gluten
- Mood changes after eating certain foods
Food Allergy Prevention: Allergen Avoidance
Once your baby has a confirmed food allergy, your allergist will help you make a clear and simple prevention and treatment plan. The most important part of this plan is avoiding the food that causes the allergy. This means learning how to:
- spot the problem food on labels
- ask questions when eating out
- be careful about cross-contact with other foods
Food allergy management also means being prepared in case your baby is accidentally exposed to a food allergen. Your allergist will teach you what symptoms to watch for and when to use epinephrine for emergency care, along with best practices for storing and using epinephrine to treat anaphylaxis. Working closely with your allergist can help you feel confident and supported.
How to avoid allergens:
- Read food labels every time – ingredients can change without warning.
- Check ingredients for common allergens that may be listed under a different name (like “casein” for milk or “albumin” for egg).
- Watch for advisory warnings like “may contain” or “made in a facility with”.
- Clean surfaces and utensils with soap and water to prevent cross-contact.
- Wash hands with soap and water (hand sanitizer doesn’t remove allergens).
- Avoid bulk bins and deli counters where scoops and slicers are shared.

Reading Food Labels to Identify Allergens
Reading food labels on baby food packages is vital in food allergen prevention. Food manufacturers are required by law to identify major allergens on all food products. This helps parents and caregivers recognize and avoid foods that could trigger allergic reactions in babies.
Where to check for allergens
- Ingredients list (look for allergen names and hidden terms)
- Contains statement (bold text like “Contains: Milk, Egg, Wheat”)
- Advisory warnings (“may contain,” “made on shared equipment”)
Read labels every time you buy a food product since ingredients can change without notice. Different package sizes may have different ingredients. Also, the same product sold in various countries may have different ingredients.
Different names for common allergens (should this be a table?)
Learn the many different names for common allergens:
- Milk: casein, whey, lactose, butter fat, ghee
- Egg: albumin, ovalbumin, globulin, livetin
- Peanut: arachis oil, groundnut, beer nuts
- Tree nuts: marzipan (almond), filbert (hazelnut)
- Soy: edamame, lecithin, tofu, tempeh, miso
- Wheat: durum, semolina, spelt, farina, graham flour
- Sesame: tahini, benne, gingelly
Preventing Cross-Contact with Food Allergens
Cross-contact happens when an unsafe food allergen accidentally comes into contact with or transfers to safe food. Even a tiny amount in a food can cause a severe allergic reaction.
Cross-contact could occur from dipping a knife in the jelly jar after it was used to spread peanut butter. Or it could happen from using the same pan to cook a hamburger after it was just used to cook shellfish.
How to prevent cross-contact
In the kitchen:
- Wash hands with soap and water before preparing food. (Commercial hand wipes are also effective. Studies show hand sanitizers are not.)
- Clean surfaces, cutting boards and utensils with soap and water.
- Use separate tools for allergen-free foods.
- Prepare safe foods first, then clean before making other foods.
When shopping:
- Avoid bulk bins where scoops are shared.
- Avoid deli counters where slicers are used for multiple products.
At restaurants:
- Ask how food is prepared.
- Request clean surfaces and utensils.
- Bring a chef card listing your child’s allergens.
- Avoid buffets or cafeterias, which have a greater risk of cross-contact due to shared utensils and spilled foods.
Create an Allergy and Anaphylaxis Emergency Plan
Work together with your allergist to create a clear Allergy and Anaphylaxis Emergency Plan that you can share with everyone who cares for your baby. The plan should include:
- Foods to avoid: a list of your baby’s specific food allergens.
- Emergency contacts: when to call 911 or go to the nearest emergency room.
- Medicine use: when and how to give epinephrine or other prescribed medicines.
- Emergency steps: how to spot a reaction and what to do first.

Epinephrine for Babies and Toddlers: First-Line Treatment for Anaphylaxis
Epinephrine is the first line of treatment for a severe allergic reaction (anaphylaxis). Knowing when and how to use epinephrine can protect your baby’s breathing, heart, and overall safety.
Signs of a serious reaction in infants can vary based on the child. It may include skin hives, trouble breathing, wheezing, trouble swallowing, swelling of the face or lips, or a hoarse/weak cry or voice. If these symptoms occur, epinephrine should be given right away and emergency care should be contacted.
Epinephrine auto-injectors are approved for young children with dose options based on a child’s weight. AUVI-Q is approved for babies as small as 16.5 pounds. Other epinephrine auto-injectors start at a dose of 33 pounds. Your child’s pediatrician will prescribe the right product and give you instructions on how to use it. (Other epinephrine products, such as a recently approved nasal spray, are not yet approved for infants.)
Parents of children at risk for anaphylaxis should always have two epinephrine doses available. In some reactions, a second dose may be needed. Talk with your child’s doctor if you should take your baby to the hospital or ER after epinephrine is given, and consider resources that explain what anaphylaxis is and when to use epinephrine to build your confidence.
When to give epinephrine:
If your baby has a known food allergy or is at risk for a serious allergic reaction, it’s vital to know when to use epinephrine. It’s always better to give epinephrine early than to wait too long.
Give epinephrine right away if your baby…
- shows severe symptoms affecting one or body symptoms after eating a food
- shows mild symptoms in more than one body system after eating a food
Body systems include the skin, respiratory system, digestive system and the heart. Look for symptoms such as hives on the skin, trouble breathing, swelling of the lips, tongue or throat, a hoarse or weak cry, pale or bluish skin, limpness or extreme sleepiness. Vomiting or diarrhea along with other symptoms can also be a sign of anaphylaxis.
If you are unsure of your child’s symptoms or their severity, remember it is safer to use epinephrine than to wait. Epinephrine works best when given early. After giving it, your baby may need medical care, even if symptoms improve. Always follow your child’s anaphylaxis action plan.
Keep two doses of epinephrine available. Sometimes symptoms come back or worsen after the first dose. It can occur hours after the initial reaction, even without additional allergen exposure. A second dose may be needed. If you administer a second dose, you should take your baby to the hospital or emergency department for follow-up treatment.
How to use an epinephrine auto-injector:
- Lay your baby down or hold them in your lap with legs extended.
- Remove the auto-injector from its case.
- Inject the epinephrine into the outer thigh muscle. Press it firmly. (You can inject through clothing.)
- Hold the auto-injector in place for 3-10 seconds, or follow the device instructions.
- Do not stand or carry your baby upright when giving the medicine. This can cause a sudden drop in blood pressure.
- The medication works within minutes.
If you’re unsure how to use the device, ask your healthcare provider for a demonstration. Most auto-injectors come with a trainer device so you can practice and feel confident.
During the anaphylaxis episode, keep your baby lying down, with legs raised if possible. This can help the blood flow back to the heart and vital organs. If your baby is vomiting or having trouble breathing, hold the body upright or turn on the side.
When to seek emergency care:
All cases of anaphylaxis should be treated with epinephrine. But not all allergic reactions require emergency care. Call 911 or go to the hospital if:
- Your baby’s allergic reaction is severe.
- Symptoms return or worsen after the first dose of epinephrine.
- Symptoms don’t go away completely after the first dose.
- A second dose of epinephrine is needed.
- You don’t have epinephrine available.

Daily Strategies for Managing Food Allergies
When your child has a serious food allergy, you may need to make some changes to your daily routine. It’s important to control your baby’s contact with allergenic foods. Your goal is to keep your child safe while allowing them to live a full, happy, and active life, and practical podcasts on managing food allergies from baby to preschool can offer day-to-day strategies.
Managing food allergies can feel overwhelming at first, but there is plenty of support for prevention and help if an allergic reaction occurs.
At home:
- Create allergen-free zones or clearly separate allergen-containing foods.
- Label safe foods with colored stickers (green for safe, red for allergens).
- Post allergy information in the kitchen for babysitters and guests.
- Reduce risk by preventing cross-contact and teach safe habits to other caregivers.
- Keep epinephrine in an easy-to-reach place. Be prepared with an emergency plan and epinephrine at all times.
- Support normal growth and development without unnecessary food limits
At daycare or school:
Planning ahead with written procedures and staff training helps create a safer environment for your child, and step-by-step guides on planning for school with food allergies can support these conversations.
- Provide written allergy plan to all staff.
- Supply clearly labeled epinephrine products.
- Confirm if staff is trained on how to recognize reactions and use epinephrine.
- Provide safe snacks for backup situations.
At restaurants:
Many families successfully eat out by partnering with knowledgeable restaurant staff and following best practices for managing food allergies while dining out.
- Call ahead to discuss your child’s allergies.
- Bring a chef card listing allergens.
- Ask about preparation methods and cross-contact prevention.
- Wipe tables and highchairs before your child sits down.

When to See a Pediatric Allergist
You should see a pediatric allergist if your baby or toddler has:
- Had a severe allergic reaction (anaphylaxis).
- Has eczema that’s hard to control.
- Needs help introducing allergenic foods safely.
- Has a diagnosed food allergy and you want to learn about management and treatment options.
A registered dietitian may also be part of your child’s care team, especially for children with complex food allergies.
What does a pediatric allergist do?
A pediatric allergist can:
- Conduct allergy testing (skin prick tests, blood tests).
- Supervise oral food challenges.
- Create a personalized food allergy management plan.
- Prescribe or refill epinephrine. (Be sure you’re aware of expiration dates.)
- Provide an anaphylaxis action plan or update an existing one as your child grows.
- Discuss treatment options like oral immunotherapy or biologics.
Can Babies Outgrow Food Allergies?
Some babies can outgrow allergies to milk, egg, or wheat by age 3-5. Your child’s allergist will help you determine if the food allergy is going away by…
- Monitoring IgE levels over time.
- Conducting oral food challenges when appropriate.
Allergists can also help you safely reintroduce foods into your child’s diet once it’s confirmed your child has outgrown the food allergy.
Peanut, tree nut, soy, fish and shellfish allergies are more likely to continue into adulthood, but some children do outgrow them.
Can Babies be Allergic to Breast Milk?
Many parents worry their baby might be allergic to breast milk, but a true allergy to human breast milk itself is extremely rare. Breast milk is usually the safest and healthiest food for babies. But some babies may react to proteins from foods the parent eats that pass into the breast milk in very small amounts.
For example, if a nursing parent eats cow’s milk, soy, eggs, or other common allergens, tiny bits of those food proteins can enter the breast milk. A baby who is sensitive or allergic to one of those proteins may then show symptoms.
This type of reaction is usually called a food protein sensitivity or a milk protein intolerance. It is not a true IgE food allergy to breast milk itself. Many babies outgrow these sensitivities as their digestive system matures.
If you think your baby is reacting to something in your breast milk, don’t stop breastfeeding on your own. Talk with your pediatrician or an allergist. They can help figure out what’s causing the symptoms and guide you on safe feeding choices.

Treatment Options for Food Allergies
If your baby develops a food allergy, therapies are available to help. They can help your baby’s body to better tolerate allergenic foods in case of an accidental exposure.
There is currently no cure for food allergies, but there are two FDA-approved food allergy medications. A third type involves baking milk and egg products.
Oral immunotherapy (OIT)
Food allergy OIT helps the body gradually get used to a food allergen. It involves giving tiny amounts of the food allergen, gradually increasing it over time until a maintenance dose is reached. The goal is to make the immune system less likely to cause an allergic reaction in case your child accidentally consumes a food allergen.
Food allergy OIT must only be done with a trained healthcare provider. Do not attempt it on your own. It is usually done at special allergy centers that have experience with this therapy.
Types of OIT:
- Palforzia® is currently available as a peanut allergy treatment but it is going to be discontinued on July 31, 2026. Since Palforzia is intended for long-term use, your doctor may no longer prescribe it. Palforzia is the first FDA-approved food allergy OIT. It is prescribed to children ages 1-17 with a peanut allergy. Palforzia comes as a capsule that comes as a special peanut protein powder that you can spread over food. It helps build tolerance to peanut. The therapy can reduce the risk of a severe reaction if a child eats a peanut product by accident, but it does not cure the allergy.
- Clinic-based OIT (not FDA-approved). Some allergy practices offer OIT for other common food allergens, such as cow’s milk, egg or tree nuts. The process is the same: your child is given small, increasing amounts of the food allergen until a maintenance dose is reached.
Biologics
Omalizumab (Xolair**®**) is FDA-approved for children 1 year and older with food allergies. It blocks IgE to reduce allergic reactions in case of accidental exposure, and recent FDA approval highlights its role as the first treatment to reduce risk of food allergy reactions.
Omalizumab is given as an injection to treat food allergy. It works by blocking the IgE that plays a major role in allergic reactions. By lowering IgE, omalizumab can help calm the immune system and reduce the severity of an allergic response from an accidental exposure.
Allergists may recommend combining omalizumab with OIT. This is called adjunct therapy. It is not FDA-approved, but research shows it is effective for children with severe or multiple food allergies. Using both treatments can:
- Improve desensitization
- Reduce allergic reactions
- Support adhering to the treatment plan
Omalizumab does not cure food allergies. Your child will still need to avoid allergens and carry epinephrine for emergencies.
Another option: baked milk/egg protocols
Some children with milk or egg allergies can safely eat those foods when they are baked at very high heat, like in muffins or bread. Baking changes the food in a way that makes it easier for some children’s bodies to handle. This does not mean the allergy is gone, but it may allow your child to eat certain baked foods without a reaction.
Your allergist may suggest using a milk ladder or egg ladder. This is a step-by-step plan that starts with baked foods and slowly moves to less-cooked forms. Each step is done carefully and only when it’s safe for your child. Over time, this may help your child’s body get used to the food. It is not a cure for milk and egg allergies, but it can lower the chance of strong reactions.
Always follow your allergist’s instructions and never try new foods without medical guidance. Even if using a ladder, you should have epinephrine nearby in case of a serious reaction.
Questions & Answers (Q&A) About Food Allergies and Young Children:
From diagnosis to treatment, food allergies can be overwhelming for many parents. Here are some questions we are frequently asked about food allergies in infants and toddlers. Always seek the advice of a medical professional for specific advice on your baby’s health. If there’s a question you’d like to see answered here, please email our editor.
April 2026
Reviewed by:
William E. Berger, MD, FACAAI, is a board-certified allergist and immunologist who serves as a media spokesperson and Chair of the Medical Advisory Council for Allergy & Asthma Network. He is a Distinguished Fellow and Past President (2002-03) of the American College of Allergy, Asthma & Immunology (ACAAI).