Food Allergy Symptoms: Mild vs. Serious
Published: March 9, 2026

When people think of food allergy symptoms, they often picture sudden, dramatic and severe reactions. But not all food allergy symptoms are severe. In fact, many people experience mild food reactions.
How do you know if you or a loved one is experiencing a mild food reaction vs. a severe food reaction? A recent survey found that 44% of parents and caregivers of children with food allergies did not understand the difference between mild and severe reactions.
First, let’s define both.
- A mild reaction is mostly localized and affects one body system. Symptoms may involve some hives on the skin or flushing. You might cough or have a runny nose or hoarse voice. Your stomach might feel upset or bloated. These symptoms are uncomfortable, but they are not life-threatening. They do not require emergency medical treatment. Your doctor may advise you take an antihistamine to treat mild symptoms.
- A serious allergic reaction is anaphylaxis, which can be life-threatening. It usually affects two or more body systems, although it can sometimes affect one body system if symptoms are severe. A serious reaction can happen when someone with a food allergy consumes a food allergen, such as a tiny bit of peanut butter in a cookie. Severe symptoms can include widespread hives, mouth or throat swelling, nausea, vomiting, and difficulty breathing. Emergency medical treatments are often necessary for serious allergic reactions.
The first line of treatment for a serious allergic reaction is epinephrine. If symptoms remain severe, worsen or come back, then you should quickly administer a second dose of epinephrine and/or go to the hospital or emergency department.
Clearing Confusion on Mild vs. Serious Food Allergies
Let’s consider two children with food allergies. Sasha is 8 years old and has an allergy to cow’s milk. She develops a few hives on the cheek when she is accidentally exposed to dairy products. The hives usually go away after a few hours. This is a mild allergic reaction.
Will is 6 years old and has a peanut allergy. He develops a rash around his mouth, sneezes, and feels nauseous. His throat swells, impacting his ability to breathe, and he feels dizzy and faint. This is a serious allergic reaction.
The reason this is important is that treatment for mild and severe allergic reactions can differ.
- For symptoms that are mild and involve just one body organ, such as a few hives on the mouth or cheek, your doctor may recommend an antihistamine. (Antihistamines are not approved for children under 2 years of age, unless specifically prescribed by the child’s doctor.)
- If symptoms are severe and involve two or more body organs, this is anaphylaxis. Use epinephrine first and fast. Any delay of epinephrine can lead to life-threatening symptoms. (Epinephrine is approved for use in young children based on the child’s weight. A dose is available for a child weighing 16.5 pounds.)
Important: even if you or your child develops mild symptoms, you should still be prepared for a severe allergic reaction. Mild symptoms can progress to severe at any time and require emergency treatment. Talk with your doctor about getting a prescription for epinephrine. Carry it at all times.
Common Food Allergens
The most common food allergies (Top 9) are caused by ingesting the following:
- cow’s milk or goat’s milk
- eggs
- peanut
- tree nuts
- wheat
- soy
- fish
- crustacean shellfish
- sesame
Mild vs. Serious Symptoms of Food Allergies
When someone eats a food to which they are allergic, the immune system overreacts. The reaction causes allergy symptoms. Symptoms can affect different organs of the body: the skin, stomach (gastrointestinal), airways and breathing (respiratory), and the heart (cardiovascular).
Each body system has telltale symptoms that suggest mild vs. serious reactions. The symptoms and the severity of the reaction will vary from person to person. When symptoms are severe, they can lead to a whole-body reaction, called anaphylactic shock.
Remember: mild symptoms typically involve one body organ, but they can turn severe without warning. Severe allergic reactions – anaphylaxis – involve two or more body organs.
Here’s what to watch for to help you determine the level of severity (for adults and children ages 4 and up):
Skin food allergy symptoms
Skin symptoms are the most common food-allergic reaction.
Mild symptoms
- A few hives around the face
- Flushing
- Itchy mouth, tongue, lips or eyes; this is a type of hives, developing under the skin
- Minor swelling of lips
Serious symptoms
- Hives that pop up and spread across different parts of the body. This shows that the allergic reaction is spreading through the bloodstream.
- Hives along with symptoms that develop in other parts of the body (respiratory, stomach or cardiovascular system).
Special cases
- Some people with allergic rhinitis may develop mild food allergy symptoms when they eat certain fruits or vegetables. These foods are linked to trees, grass or weed pollen. Common symptoms include an itchy mouth or skin irritation. This is a condition is known as Oral Allergy Syndrome (OAS). Call your physician if you notice oral allergy syndrome symptoms.
- Some people have a food intolerance or sensitivity, like lactose intolerance. This is not a true food allergy. But they can make eating certain foods hard. It’s important to see an allergist for food allergy of food intolerance testing.
Gastrointestinal food allergy symptoms
Stomach symptoms are particularly common among young children.
Mild
- Stomach discomfort
- Bloating
- Slight nausea
Serious:
- Vomiting
- Severe pain or cramping
- Severe nausea
- Diarrhea
Respiratory food allergy symptoms
Respiratory symptoms related to food-allergic reactions are often serious. This is especially true for people who have both asthma and food allergies.
Mild
- A slight cough
- A slightly hoarse voice
- Runny nose
Severe
- Wheezing
- Shortness of breath or chest tightness
- Tightness in the throat
- Swelling of the mouth, tongue or throat that interferes with breathing or swallowing. Usually these symptoms involve a person with a history of severe food allergy reactions.
- Severe or uncontrollable cough
- A very hoarse voice
Special cases
- Respiratory symptoms are serious for people with asthma. If coughing, wheezing, shortness of breath or chest tightness occur after eating food, use epinephrine first, not a quick-relief albuterol inhaler. Epinephrine helps breathing, whether the cause is a food allergen or an asthma trigger. Fatal anaphylaxis cases have happened in people with both food allergies and asthma. Don’t hesitate to use epinephrine.
Cardiovascular (heart) food allergy symptoms
Cardiovascular symptoms are always serious and usually require immediate treatment. Use epinephrine and call 911.
Serious
- Dizziness, fainting, or changes in blood pressure. This indicates decreased blood pressure and blood flow to the brain.
- Pale skin, blue-tinged lips or fingernails. This indicates restricted oxygen and blood flow throughout the body.
Neurologic (behavioral) food allergy symptoms
Neurologic symptoms are also always serious and are usually combined with other symptoms of food allergy.
Serious
- Confusion
- A feeling of impending doom
- Agitation
- Altered consciousness
Mild vs. Serious Allergic Reactions At-a-Glance
| Mild Allergic Reactions | Serious Allergic Reactions |
|---|---|
(typically involves 1 body system) | (involves 2 or more body systems or 1 body system with severe symptoms – this is anaphylaxis) |
• Few hives • Mild swelling of the lips • Flushing • Itchy mouth, tongue, lips, or eyes • Slight cough • Runny nose • Slightly hoarse voice • Stomach discomfort • Slight nausea • Bloating | • Widespread hives • Swelling of the mouth, tongue or throat that interferes with breathing or swallowing. • Wheezing • Shortness of breath or chest tightness • Severe or uncontrollable cough • A very hoarse voice • Vomiting or diarrhea • Severe abdominal pain or cramping • Severe nausea • Changes in blood pressure • Pale skin; blue lips or fingernails • Fainting or dizziness • Confusion • Agitation • Feeling of impending doom |
Food allergy symptoms in infants and toddlers
Mild and serious allergic reactions can occur in infants (first year of life) and toddlers (ages 1-3). Just like in older children and adults, mild symptoms typically involve one body system while anaphylaxis involves two or more body systems.
However, infants and toddlers may have food allergy symptoms that are more challenging to detect. This is due in part to their inability to verbalize what they are feeling.
Infants and toddlers may have unique ways of showing they are experiencing an allergic reaction. For example, some may rub their skin to indicate swelling or hives. They might arch their back to suggest stomach discomfort. They may show rapid breathing or belly breathing to indicate respiratory issues. Some might have a weak pulse, limp body or poor head control, suggesting cardiovascular problems.
Check out the Recognizing Anaphylaxis in Infants and Toddlers infographic. It reviews the unique signs and symptoms of serious food allergy reactions in young children.
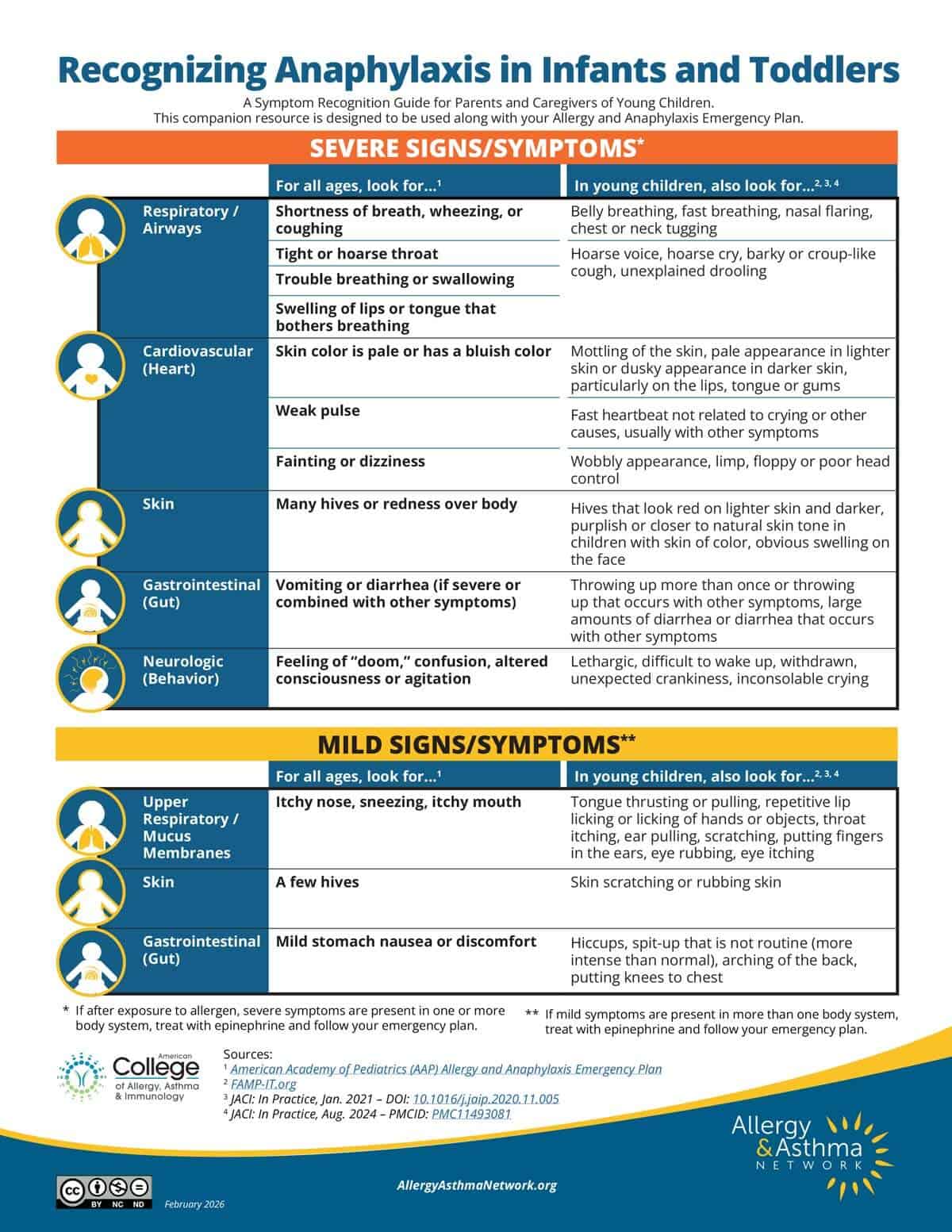
Visit our online store to download our free Recognizing Anaphylaxis in Infants and Toddlers
Learn more about infant anaphylaxis, from identifying symptoms to treatment.
Managing and treating mild and severe food allergies
Even if you tend to have mild food allergy symptoms, it’s best to stay away from any food to which you are allergic. This is because there’s no way to predict the severity of a reaction from one day to the next. Mild reactions can turn severe at any time.
Food allergen avoidance is essential. Check ingredients and read food labels for most food allergies, particularly the Top 9. Find out if safe food substitutions are available.
Open communication of food allergies is very important to help manage food allergies. Alert wait staff and, if possible, chefs when going out to eat at restaurants. For schoolchildren, meet with school nurses and teachers to discuss food allergies and emergency protocols.
If you don’t know the food allergen that is causing symptoms, see an allergist for testing. Following a positive food allergy diagnosis, ask your allergist for a written Allergy and Anaphylaxis Emergency Plan. This has specific instructions about what to do if symptoms occur.
For treatment of a mild allergic reaction, your doctor may prescribe antihistamines. Antihistamines are not indicated for children under the age of 2 unless specifically prescribed by the child’s doctor.
For severe food allergy reactions, epinephrine is the first-line treatment. Epinephrine is approved for use in young children based on the child’s weight. The minimum weight is 16.5 pounds for a dose of epinephrine.
Food allergy therapies
Therapies for food allergyinclude oral immunotherapy (OIT) and a biologic medication. OIT can be used to treat mild, moderate or severe food allergies. The biologic – omalizumab (Xolair®) – is for moderate-to-severe food allergies.
What is oral immunotherapy? It starts with a tiny amount of a food allergen, then gradually larger amounts until a target dose is reached. This helps desensitize the patient to the food allergen and protects against an accidental exposure. OIT can be used to prevent both mild and severe allergic reactions.
OIT should only be done in a medical setting such as an allergist’s office. Do NOT attempt it on your own. The only FDA-approved OIT is for peanut allergy and it is called Palforzia®. The treatment is for children ages 1-17. Palforzia is not meant to cure peanut allergies. Rather, it is to help reduce the frequency and severity of peanut allergy symptoms in case of an accidental exposure.
Allergists who specialize in food allergy may also offer office-based oral immunotherapy for peanut and other food allergens such as dairy.
The biologic omalizumab (Xolair®) is FDA-approved to treat moderate-to-severe food allergies. It targets and blocks the Immunoglobulin E (IgE) antibody. IgE is a driver of food-allergic reactions. Reducing levels of IgE keeps the body from reacting to an allergen.
Xolair is given as a injection every 2-4 weeks. It allows people who are at risk for severe food-allergic reactions (anaphylaxis) to tolerate an accidental exposure to a food allergen. Xolair also reduces the risk of an allergic reaction.
Reviewed by:
Purvi Parikh, MD, FACAAI, is an adult and pediatric allergist and immunologist at Allergy and Asthma Associates of Murray Hill in New York City. She is on faculty as Clinical Assistant Professor in both departments of Medicine and Pediatrics at New York University School of Medicine.










