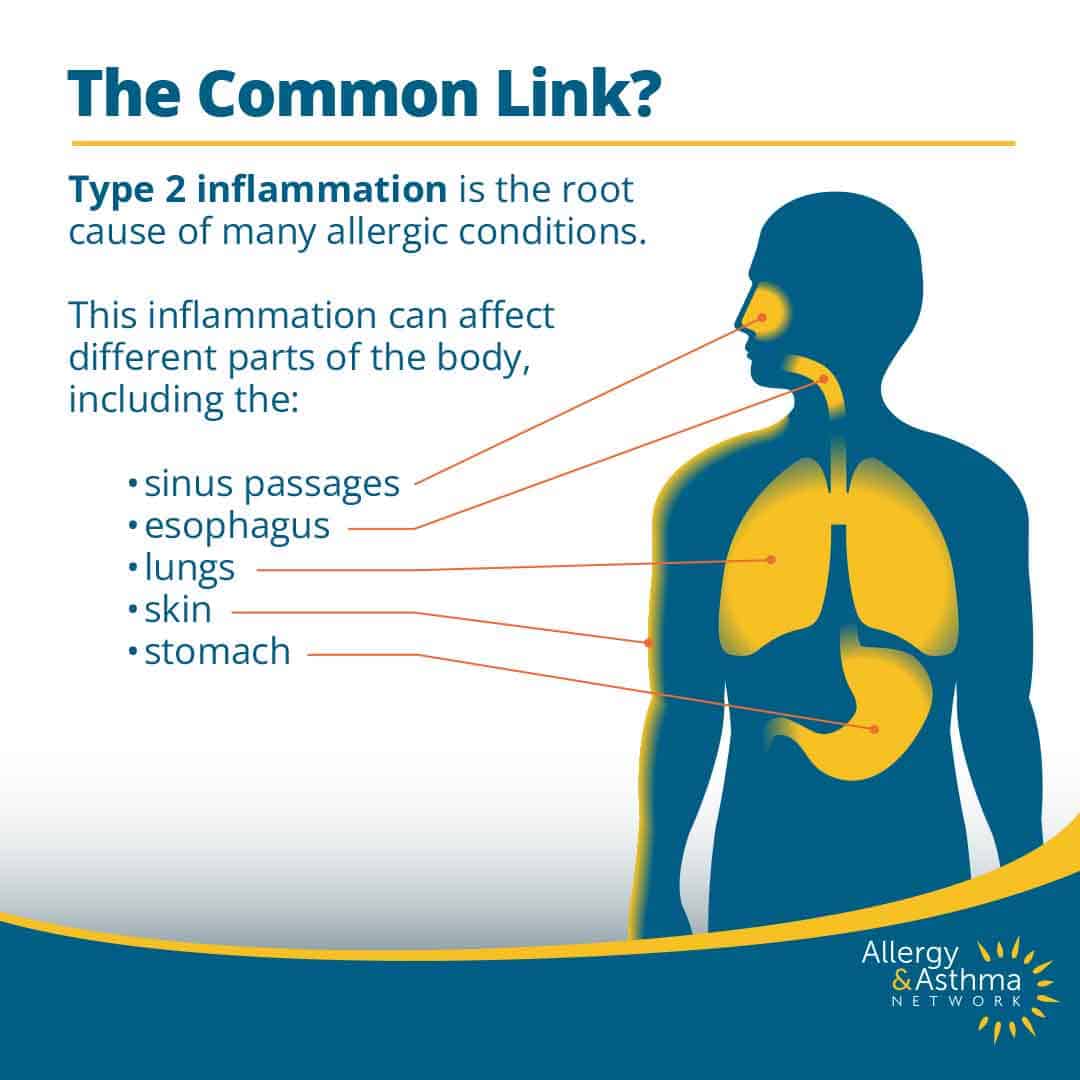
What is Type 2 Inflammation?
Type 2 inflammation is an overactive immune response that causes excess inflammation in the body. It plays a significant role in severe and sometimes chronic diseases. These include respiratory, skin and atopic diseases, including asthma, allergies and eczema (atopic dermatitis). It is often triggered by allergens but can also arise from other irritants or infections. Genetics may play a role as well.
In allergic reactions, the immune system produces immunoglobulin E (IgE) antibodies. These bind to immune cells such as mast cells and basophils. This interaction triggers the release of histamine and inflammatory cytokines (proteins). The primary cytokines involved in respiratory, skin and allergic diseases are interleukin-4 (IL-4), IL-5 and IL-13. They can cause Type 2 allergic inflammation.
Type 2 inflammation can also be driven by high levels of eosinophils, a type of white blood cell. The same cytokines recruit and activate the eosinophils. This causes inflammation in the airways or skin. Chronic inflammation can lead to long-term symptoms and tissue damage if not well-managed.
What causes Type 2 inflammation?
People with allergic, respiratory and skin conditions often have some Type 2 inflammation. Environmental and genetic factors appear to play a role.
Type 2 inflammation arises when the immune system overreacts to triggers like allergens, irritants, or infections. This overreaction involves a cascade of immune responses. This includes the production of cytokines and activation of inflammatory cells like eosinophils. While this response is meant to protect the body, it can lead to chronic diseases when it becomes uncontrolled or excessive.
Health conditions that may be affected by Type 2 inflammation include:
- Moderate to severe asthma
- Eosinophilic asthma
- COPD
- Aspirin-Exacerbated Respiratory Disease (AERD)
- Allergic rhinitis
- Severe chronic rhinosinusitis with nasal polyps (CRSwNP)
- Chronic urticaria (chronic hives)
- Moderate to severe atopic dermatitis (eczema)
- Food allergies
- Eosinophilic esophagitis (EoE)
Type 2 inflammation is believed to be the underlying cause of these conditions. It could also be the reason the condition is hard to control or why someone may have more than one of these conditions.
Healthcare providers can diagnose Type 2 inflammation through testing. These tests measure your blood eosinophil levels and blood IgE levels. There are also breathing tests for your lungs called fractional exhaled nitric oxide (FeNO).
Treatment options are available for people with diseases impacted by Type 2 inflammation. Biologic medications are increasingly prescribed to treat conditions worsened by Type 2 inflammation.
Work with your healthcare provider to decide what course of treatment is best for you. Consider the severity of your symptoms. Discuss what previous medications/treatments you have tried. Find out if Type 2 inflammation is related to any other medical conditions you may have.

Asthma and Type 2 inflammation
Type 2 inflammation is a major driver of moderate to severe asthma. It affects between 55% to 70% of adults with severe asthma. It is characterized by the release of proteins IL-4, IL-5 and IL-13. These increase IgE levels and activate immune cells like mast cells and eosinophils.
When asthma is triggered by allergens, irritants, viruses or other exposures, it can cause inflammation in the body. The response activates immune cells, releasing inflammatory mediators such as histamine. This leads to severe symptoms of coughing, wheezing, shortness of breath and chest tightness. It makes it hard to breathe.
If you have asthma with Type 2 inflammation, you may experience severe or hard-to-control symptoms. It can lead to an increased risk of asthma exacerbations and reduced lung function.
Inhaled corticosteroids (ICS) and long-acting beta2-agonists (LABA) are prescribed to asthma patients. The medications work to improve symptom control. Severe asthma is the diagnosis when these medications are not effective. Doctors then turn to different therapies, or a combination of medications, to improve symptom control. Leukotriene modifiers are drugs that block the chemicals that cause airway inflammation. Biologics target the cells that cause inflammation in the body. They can help stop symptoms before they can start.
Learn more about asthma

Eosinophilic asthma and Type 2 inflammation
Eosinophilic asthma is a difficult to control or severe asthma phenotype. It is sometimes referred to as eos asthma. Type 2 inflammation is a key driver of eosinophilic asthma. The condition is most common in adults, although it may occur in children and young adults.
Eosinophils are white blood cells that are activated by the release of cytokines IL-4, IL-5 and IL-13. This can lead to a surge of eosinophils in the blood, lung tissue and/or mucus (known as sputum).
Eosinophilic asthma can be triggered by respiratory infections (such as flu), air pollution, secondhand smoke, or other irritants. It is sometimes triggered by environmental allergens like pollen, mold, dust mites, or pet dander. It is possible for someone to have both allergic asthma and eosinophilic asthma.
People with severe eosinophilic asthma may experience worse symptoms of cough, wheeze, shortness of breath and chest tightness. Research shows a connection between too many eosinophils in the blood and the future risk and severity of asthma attacks.
If quick-relief and daily controller medications (such as inhaled corticosteroids) are not helping, talk with an asthma specialist. Ask about other medications. Doctors may recommend a combination of a LABA and ICS and/or a long-acting muscarinic antagonist (LAMA). Leukotriene modifiers are drugs that block chemicals that cause inflammation in the airways. Biologics are specialized medications to treat eosinophilic asthma. They can reduce eosinophils in the blood, stopping symptoms before they can start.
Learn more about eosinophilic asthma
➤ What is eosinophilic asthma?

COPD and Type 2 inflammation
Chronic obstructive pulmonary disease (COPD) is a long-term disease caused by damaged lungs. The disease causes severe symptoms of coughing, wheezing and shortness of breath. It usually happens because of smoking, air pollution, or sometimes family history. Type 2 inflammation is not a primary driver for most COPD cases. However a subset of COPD patients with high eosinophil levels may experience Type 2 inflammation.
Eosinophils are white blood cells that can trigger Type 2 inflammation in the airways. When activated by the release of cytokines, they can cause an increase of eosinophils in the blood, lung tissue and/or mucus. Symptoms may be triggered by smoking or a respiratory virus or the flu.
Type 2 inflammation in people with COPD can make the lungs more swollen, increasing the risk of flare-ups. Some people with COPD and Type 2 inflammation may also have symptoms similar to asthma, a condition called Asthma-COPD Overlap.
Knowing if someone with COPD has Type 2 inflammation can help doctors choose the right treatment. They may prescribe medicines that reduce inflammation to help prevent flare-ups and make breathing easier. LABAs and LAMAs can help with COPD control. There is a biologic medication approved to treat adults with poorly controlled COPD and an eosinophilic phenotype. It can help stop or reduce eosinophilic inflammation. It can also reduce eosinophils in the blood.
Learn more about COPD

Aspirin-exacerbated respiratory disease (AERD) and Type 2 inflammation
AERD, also known as Samter’s Triad, is a chronic inflammatory disease that involves:
- asthma
- recurrent nasal polyps (soft, teardrop-shaped, non-cancerous, painless growths in the sinuses)
- a sensitivity to aspirin and/or other non-steroidal anti-inflammatory drugs (NSAIDs)
Type 2 inflammation plays a key role in asthma and inflamed airways. It also plays a key role in nasal polyps related to chronic rhinosinusitis. AERD patients with Type 2 inflammation may experience severe asthma symptoms, sinus congestion and nasal polyps.
If you are diagnosed with AERD and your symptoms are not getting better, talk with your doctor or find a specialist. Medications for severe asthma and nasal polyps are available. These may include inhaled corticosteroids, corticosteroid nasal sprays and biologics that treat the source of symptoms.
Learn more about AERD

Allergic rhinitis and Type 2 inflammation
Allergic rhinitis (also called hay fever) is defined as “inflammation of the nose.” It is the body’s reaction after exposure to allergens such pollen, mold, dust mites or animal dander. IgE antibodies produce the cytokines IL-4, IL-5 and IL-13. This releases histamine and causes Type 2 inflammation. It can cause sneezing, inflamed nasal passages, a runny or stuffy nose, itchy eyes, and throat irritation.
Type 2 inflammation can make allergic rhinitis symptoms worse. It can cause swelling and mucus. Over time, the inflammation can make the immune system even more sensitive to allergens.
Treatments for allergic rhinitis often aim to control Type 2 inflammation. Antihistamines block the effects of histamine and reduce symptoms. Nasal corticosteroids reduce inflammation in the nasal passages.
Biologics are not indicated to treat allergic rhinitis. But they are approved for allergic asthma and CRSwNP. Some may be effective in treating allergic rhinitis because it can reduce IgE levels. This helps prevent the release of histamine that can cause or worsen allergic rhinitis.
Some people with allergic rhinitis are helped by allergen immunotherapy.
Learn more about allergic rhinitis

Chronic rhinosinusitis with nasal polyps (CRSwNP) and Type 2 inflammation
Chronic rhinosinusitis with nasal polyps (CRSwNP) involves inflamed sinus and nasal cavities. Research shows as many as 85% of CRSwNP cases are associated with Type 2 inflammation. Many people diagnosed with CRSwNP may also have asthma or allergic rhinitis.
In CRSwNP, the immune system responds to allergens, irritants or infections. (Not all triggers are clear and obvious, however.) The release of cytokines IL-4, IL-5 and IL-13 in the body activate eosinophils in the blood. This can cause Type 2 inflammation and increased mucus in the sinus and nasal passages.
When there is inflammation in the nose, it can become a breeding ground for nasal polyps. This can lead to worsened CRSwNP symptoms: nasal congestion, postnasal drip and difficulty breathing through the nose. It can also lead to frequent sinus infections.
CRSwNP treatment options include corticosteroid nasal sprays, a short course of oral corticosteroids, and possibly surgery if nasal polyps are large. If corticosteroids are not helpful, biologics are approved to treat CRSwNP. Several biologic medications target the eosinophils that cause inflammation.
Talk with an allergist about your symptoms and treatment options.
Learn more about CRSwNP
➤ What is Chronic Rhinosinusitis with Nasal Polyps (CRSwNP)?

Chronic Urticaria and Type 2 inflammation
Chronic urticaria refers to hives that persist for six weeks or longer. These raised, itchy, inflamed welts can appear anywhere on the body and may be painful. They may sometimes occur after exposure to an allergen, irritant or infection. Exposure to sunlight, cold temperature, exercise and skin friction are also potential triggers. This activates IgE and releases the histamine that causes symptoms. Chronic idiopathic urticaria (CIU), also known as chronic spontaneous urticaria (CSU), occurs without an obvious trigger.
Research into what drives chronic urticaria is ongoing. It is a disease driven by mast cells and IgE-mediated histamine release. Recent studies suggest Type 2 inflammation involving cytokines IL-4, IL-5 and IL-13, may play a key role in chronic urticaria, especially people with elevated IgE or eosinophil levels.
Antihistamines are the first line of treatment for chronic urticaria. If they don’t work, then your doctor may consider other medications, such as biologics. Biologics may keep IgE from binding with cells, preventing histamine release. They can help stop symptoms before they can start and reduce the number of hives and their severity. Talk with an allergist or dermatologist to find the right treatment for you.
Learn more about chronic urticaria
➤ Chronic urticaria: causes, symptoms, treatment
➤ Chronic urticaria management and resources

Eczema and Type 2 inflammation
Eczema is a chronic inflammatory skin condition. (Atopic dermatitis is a form of eczema). It causes dry, itchy, scaly, inflamed patches of skin. Eczema can affect people of all ages, but it is especially common in children. The condition often comes and goes in flares, and its root cause involves genetics and environmental factors.
Type 2 inflammation driven by the cytokines IL-4 and IL-13 is a key contributor to moderate to severe eczema. These proteins cause histamine and lead to high levels of eosinophils. They contribute to severe skin inflammation and tissue damage.
Topical corticosteroids and other medicated ointments are often prescribed first to treat eczema. Specialized medications can help inhibit Type 2 inflammation. JAK inhibitors stop or reduce the inflammation. They limit proteins that cause allergic reactions and inflamed skin. Several biologics treat moderate to severe eczema. These biologics block the proteins that cause symptoms. They stop inflammation before it can start.
If you have severe or worsening eczema, talk with an allergist or dermatologist. Work together to find the right treatment for you.
Learn more about eczema
➤ What is Moderate to Severe Eczema

Food allergies and Type 2 inflammation
A food allergy is an immune system response to a certain food. The top 9 food allergens are peanut, tree nuts, egg, cow’s milk, soy, wheat, fish, shellfish and sesame. Some other foods may also cause an allergic reaction.
Type 2 inflammation plays a key role in food-allergic symptoms. When you ingest a food allergen, your body reacts by producing the antibody immunoglobulin E (IgE). This triggers the release of histamine, causing a host of symptoms, including Type 2 inflammation. Symptoms may include hives on the skin, swelling in the mouth, throat and airways and difficulty breathing. High levels of eosinophils may also cause symptoms, particularly digestive problems.
Most people with food allergies are advised to avoid their food allergen(s). But accidental exposures can occur. Food-allergic reactions are potentially life-threatening and may require emergency treatment. Epinephrine is the first-line treatment for a severe allergic reaction, or anaphylaxis.
There is a biologic approved for severe food allergies. The goal is to help people better tolerate an accidental food allergy exposure. The biologic blocks the IgE antibody that drives food-allergic reactions. This can help prevent the body from over-reacting to an allergen and also reduce the risk and severity of allergic reactions.
Learn more about food allergies
➤ Food allergy treatment and management

Eosinophilic esophagitis (EoE) and Type 2 inflammation
Eosinophilic esophagitis (EoE) is a chronic condition involving high levels of eosinophils in throat tissue. It is associated with Type 2 inflammation and swelling in the esophagus. This can make it hard to swallow food. Symptoms also may involve reflux, chest pain and food getting stuck in the throat.
EoE can affect people of all ages, including infants. Symptoms tend to vary among age groups. They are sometimes caused by allergic reactions to food or environmental allergens.
EoE is treated by modifying the diet to avoid trigger foods and medications. Swallowed corticosteroids (liquid or oral forms) can help control inflammation in the throat.
If dietary modifications and corticosteroids do not help, there is a biologic medication approved to treat EoE. It works by blocking the proteins IL-4 and IL-13 that activate eosinophils and cause Type 2 inflammation. It can help reduce inflammation in the esophagus before it can start. It can also open up an inflamed esophagus.
Learn more about eosinophilic esophagitis
➤ Eosinophilic esophagitis: symptoms, causes, diagnosis and treatment
Reviewed by:
Bradley Chipps, MD, FACAAI, is a board-certified allergist and pediatric pulmonologist with Capital Allergy and Respiratory Disease Center in Sacramento, California. He earned his medical degree from University of Texas Medical Branch in Galveston in 1972. He is Past President of the American College of Allergy, Asthma and Immunology (ACAAI).